A nurse expertly guides patients through polyethylene glycol (PEG) bowel prep, ensuring optimal colonoscopy results and improved diagnostic accuracy, as highlighted by recent studies.
PEG solutions, often combined with ascorbic acid, demonstrate high effectiveness in cleansing the bowel, facilitating clearer visualization during colonoscopic examinations, according to Healio.
Proper preparation, including dietary adjustments and medication reviews, is crucial for successful cleansing, as emphasized in patient instructions and clinical protocols.
What is Polyethylene Glycol (PEG)?
Polyethylene glycol, often referred to as PEG, is a large molecule of polyethylene oxide commonly utilized as a bowel cleanser before colonoscopies or other intestinal procedures. It functions as an osmotic laxative, meaning it draws water into the colon, softening the stool and stimulating bowel movements to effectively clear the intestinal tract.
Unlike stimulant laxatives, PEG doesn’t directly irritate the bowel wall, making it generally well-tolerated. It’s available in various formulations, including powders that are mixed with water. The Healio reports emphasize its effectiveness when combined with ascorbic acid, enhancing bowel preparation quality.
PEG is considered safe for most individuals, but it’s crucial to follow a healthcare provider’s instructions carefully regarding dosage and timing. Proper hydration during PEG administration is vital to prevent dehydration and electrolyte imbalances. It’s a cornerstone of effective colonoscopy preparation.
Why is Bowel Cleansing Necessary?
Bowel cleansing, specifically with solutions like polyethylene glycol (PEG), is paramount for successful diagnostic procedures, most notably colonoscopies. A clean colon allows the physician to clearly visualize the intestinal lining, detecting polyps, tumors, or other abnormalities that might otherwise be obscured by fecal matter.
Effective preparation, as highlighted by resources like Healio, directly impacts the accuracy of the colonoscopy and reduces the need for repeat procedures. Inadequate cleansing can lead to missed lesions, potentially delaying crucial diagnoses and treatments.
Beyond diagnostics, bowel cleansing is sometimes necessary before certain surgeries or medical interventions. It minimizes the risk of infection and improves surgical outcomes. Thorough preparation, guided by healthcare professionals, is therefore a critical step in ensuring patient safety and optimal medical care.

Preparation Before Starting PEG Administration
Patients must receive detailed instructions regarding dietary restrictions, medication adjustments, and a thorough review of the PEG administration process for success.
Dietary Restrictions Prior to Cleansing
The nurse explains that a clear liquid diet is essential 24-48 hours before the procedure, avoiding solid foods, milk, and anything red or purple in color.
Clear liquids include broth, clear juices (apple, white grape), water, plain tea, and clear gelatin (without fruit). Patients should avoid dairy, red or purple dyes, and any solid food particles.
The nurse emphasizes the importance of adhering strictly to these guidelines to ensure effective bowel preparation. Consuming prohibited items can compromise the colonoscopy’s accuracy.
Patients with diabetes should discuss dietary modifications with their healthcare provider to manage blood sugar levels during the clear liquid diet phase. Hydration with clear liquids is also crucial to prevent dehydration.
The nurse reinforces that complete adherence to the dietary restrictions is paramount for a successful and informative colonoscopy.
Medication Considerations
The nurse meticulously reviews the patient’s medication list, focusing on drugs that may interfere with bowel cleansing or require adjustments during preparation;
Patients taking blood thinners, such as warfarin or aspirin, must inform their physician, as these may need temporary discontinuation to minimize bleeding risk during the colonoscopy.
Diabetic medications require careful management, as the clear liquid diet can significantly impact blood sugar levels. Dosage adjustments may be necessary, guided by the patient’s endocrinologist.
Iron supplements should be stopped several days prior, as they can darken stool and obscure visualization. The nurse stresses the importance of not altering any medication without prior medical approval.
Patients should bring a complete medication list to their appointment, and any questions regarding medication adjustments should be directed to their healthcare provider.
Reviewing the Procedure with the Patient
The nurse comprehensively explains the colonoscopy procedure, addressing patient anxieties and ensuring informed consent. This includes detailing the purpose of the exam, what to expect during the process, and potential risks.
A clear explanation of the bowel preparation process is provided, emphasizing the importance of complete cleansing for accurate results. The nurse reinforces the timing of PEG solution ingestion and dietary restrictions.
Patients are encouraged to ask questions and voice concerns. The nurse clarifies that the procedure is typically painless due to sedation, but mild cramping or bloating may occur during cleansing.
Post-procedure instructions are reviewed, including dietary resumption and potential side effects. Transportation arrangements are confirmed, as patients cannot drive after sedation.
The nurse provides written materials summarizing the information, reinforcing patient understanding and promoting adherence to the preparation guidelines.
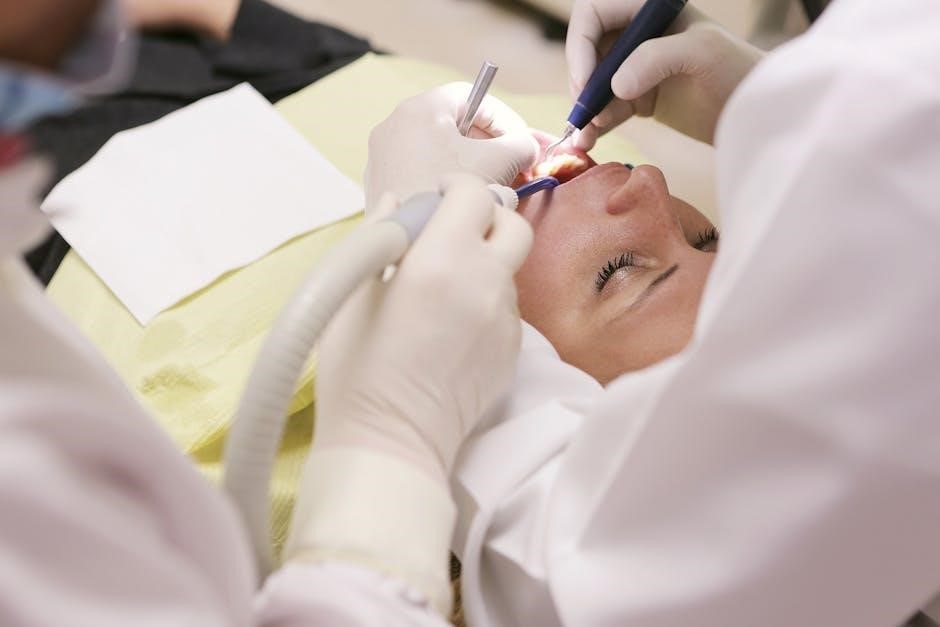
Administering the PEG Solution
Nurses carefully guide patients through mixing and consuming the PEG solution, ensuring proper dosage and timing for effective bowel cleansing before colonoscopy.
Mixing the PEG Solution
To prepare the polyethylene glycol (PEG) solution, the nurse will instruct the patient to thoroughly dissolve the entire contents of the PEG powder packet into the specified amount of water – typically one gallon or four liters.
It is crucial to use clear, potable water and to stir the mixture continuously until the powder is completely dissolved, ensuring no granules remain. This process may take approximately 15-20 minutes. The resulting solution should appear clear or slightly cloudy; any discoloration warrants contacting a healthcare professional.
Patients should be advised to mix the solution in a clean container and to refrigerate any unused portion for up to 24 hours. Proper mixing is essential for the solution’s effectiveness and patient tolerance, as undissolved PEG can hinder bowel preparation.
Dosage and Timing
The standard dosage for polyethylene glycol (PEG) bowel cleansing typically involves consuming the entire prepared solution – usually four liters – split into two equal doses. The first dose is generally administered the evening before the scheduled colonoscopy, and the second dose is taken approximately 4-6 hours before the procedure.
It’s vital to adhere strictly to the prescribed timing, as this ensures adequate bowel evacuation. Patients should be instructed to drink each half of the solution within a one to two-hour timeframe.
Pacing the consumption, rather than drinking it rapidly, can help minimize nausea and discomfort. The nurse should emphasize the importance of completing the entire regimen, even if initial bowel movements appear clear, to optimize preparation quality.
Administration Methods
Polyethylene glycol (PEG) solutions are typically administered orally. Patients are encouraged to drink the solution at room temperature, as this can improve palatability. While some individuals may tolerate the large volume easily, others might find it challenging.
To facilitate consumption, the nurse should suggest using a straw positioned towards the back of the tongue, or alternating between sips of the PEG solution and clear liquids like broth or ginger ale. For patients with difficulty tolerating the volume, smaller, more frequent sips may be recommended.
In rare cases, if oral administration is impossible, alternative methods, such as nasogastric or rectal administration, might be considered under strict medical supervision, though these are less common.
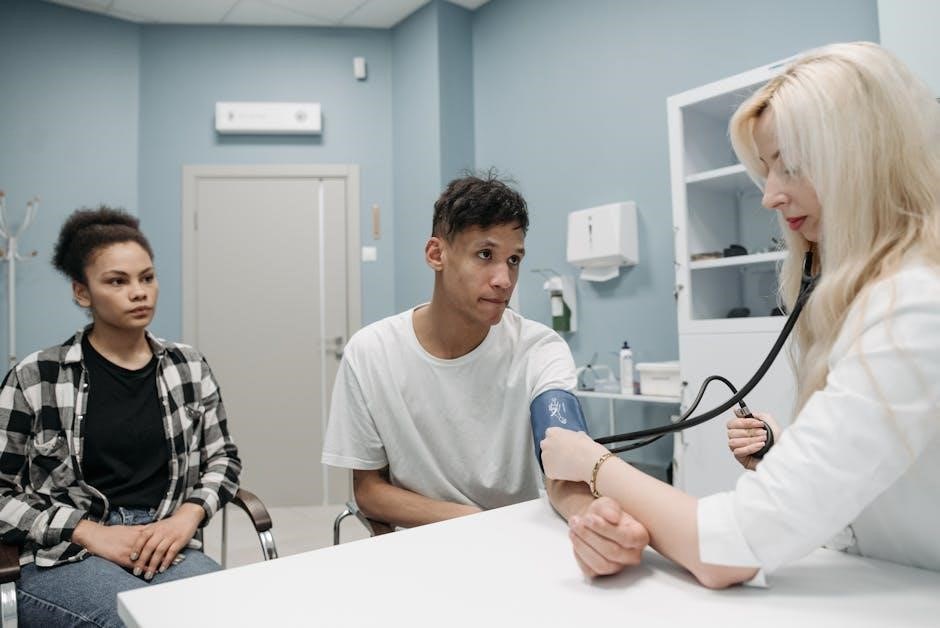
Monitoring the Patient During Cleansing
Nurses vigilantly assess bowel movement clarity, hydration status, and promptly address any adverse effects during PEG administration, ensuring patient safety and comfort.
Assessing Bowel Movements
The nurse instructs patients to carefully observe and report the characteristics of their bowel movements throughout the cleansing process. Initially, movements may contain formed stool, gradually transitioning to liquid with decreasing amounts of solid matter.
A successful cleanse is indicated by clear, yellow-tinged liquid stool, free from particulate matter. Patients should be informed that achieving this clarity is the primary goal, signifying adequate colonic preparation for the upcoming procedure.
The frequency of bowel movements will vary, but the nurse emphasizes the importance of consistent monitoring and documentation. Any deviation from the expected progression – such as persistent solid stool or a sudden cessation of bowel movements – should be immediately reported to the healthcare team for evaluation and potential intervention.
Detailed observation and accurate reporting are vital for optimizing the effectiveness of the PEG solution and ensuring a successful colonoscopy.
Monitoring for Adverse Effects
The nurse thoroughly instructs patients to vigilantly monitor for potential adverse effects during PEG administration. Common side effects, like nausea, bloating, abdominal cramping, and anal discomfort, are typically mild and self-limiting, but should be reported if severe or persistent.
More serious, though less frequent, complications include electrolyte imbalances – particularly hypokalemia – and dehydration. Patients with pre-existing cardiac or renal conditions are at increased risk and require closer observation. Symptoms of electrolyte imbalance, such as muscle weakness, irregular heartbeat, or confusion, necessitate immediate medical attention.
Maintaining adequate hydration is crucial to mitigate these risks. Patients should be advised to promptly report any signs of dizziness, lightheadedness, or decreased urine output. The nurse emphasizes the importance of contacting a healthcare provider for any concerning symptoms.
Maintaining Hydration
The nurse stresses the paramount importance of maintaining adequate hydration throughout the PEG bowel cleansing process. Due to the large-volume nature of the solution and its diarrheal effect, significant fluid loss is expected. Patients are instructed to drink clear liquids – water, clear broth, or electrolyte-containing beverages – consistently, even if they feel full.

Aim for at least 8 ounces of fluid every hour during preparation. Avoiding sugary drinks is recommended, as they can exacerbate electrolyte imbalances. The nurse clarifies that proper hydration not only prevents dehydration but also helps minimize potential side effects like nausea and cramping.
Patients should be educated to recognize signs of dehydration, including decreased urine output, dizziness, and extreme thirst, and to promptly report these to their healthcare provider. Consistent fluid intake is key to a safe and effective cleanse.

Potential Side Effects and Management
The nurse details common side effects like nausea and bloating, advising symptom management with rest and clear liquids; serious issues require immediate medical attention.
Common Side Effects (Nausea, Bloating)
The nurse explains that experiencing nausea and bloating during PEG bowel preparation is quite common, stemming from the large volume of fluid ingested and the bowel’s active cleansing process. Patients should be reassured that these symptoms are generally mild and temporary, typically subsiding as the bowel evacuation progresses.
To mitigate nausea, sipping clear liquids slowly, avoiding strong odors, and resting can be beneficial. For bloating, gentle abdominal massage and avoiding carbonated beverages are recommended. The nurse emphasizes the importance of not stopping the PEG solution unless symptoms become severe or unmanageable, as completing the full dose is crucial for adequate bowel preparation.
Patients are instructed to report persistent or worsening nausea or bloating, but understand that mild discomfort is a normal part of the process. Maintaining a calm and relaxed demeanor can also help minimize these side effects.
Serious Side Effects (Electrolyte Imbalance)
The nurse stresses the potential, though infrequent, risk of electrolyte imbalances during PEG bowel cleansing, particularly in patients with pre-existing conditions like renal impairment or cardiac issues. Excessive fluid loss through diarrhea can disrupt the delicate balance of sodium, potassium, and magnesium, leading to serious complications.
Patients are educated on recognizing symptoms of electrolyte imbalance, including muscle weakness, irregular heartbeat, confusion, and severe dizziness. They are explicitly instructed to immediately report any of these symptoms to their healthcare provider.
The nurse explains that careful monitoring of fluid intake and output, as well as potential blood tests, may be necessary to detect and correct any imbalances promptly. Pre-existing medication adjustments may also be required to minimize this risk.
When to Contact a Healthcare Provider
The nurse emphasizes the importance of promptly contacting a healthcare provider if any concerning symptoms arise during or after PEG bowel cleansing. Patients are instructed to seek immediate medical attention for severe abdominal pain, persistent vomiting, inability to tolerate fluids, or signs of dehydration like decreased urination and extreme thirst.
Furthermore, any symptoms suggestive of electrolyte imbalance – muscle weakness, irregular heartbeat, confusion, or dizziness – warrant immediate medical evaluation. The nurse clarifies that even seemingly minor concerns should be reported, as early intervention can prevent complications.
Patients are provided with clear contact information for their healthcare team and instructed not to hesitate to reach out with any questions or anxieties regarding the procedure or their well-being.

Special Considerations
Nurses tailor PEG instructions for patients with renal or cardiac issues, and the elderly, adjusting dosage and monitoring closely for adverse effects and safety.
PEG for Patients with Renal Impairment
When instructing patients with renal impairment about PEG bowel preparation, nurses must emphasize cautious hydration and meticulous electrolyte monitoring. Reduced kidney function impacts electrolyte balance, potentially leading to complications during cleansing.
Patients should be advised to consume the PEG solution slowly, as rapid administration can exacerbate fluid and electrolyte shifts. The nurse should clearly explain the importance of reporting any signs of fluid overload, such as shortness of breath or edema.
Pre-existing renal conditions necessitate a thorough assessment of the patient’s baseline kidney function and a collaborative discussion with the healthcare provider regarding potential adjustments to the PEG regimen. Post-cleansing monitoring of renal function is also crucial to ensure patient safety and prevent acute kidney injury.
PEG for Patients with Cardiac Issues
Instruction for patients with cardiac conditions undergoing PEG bowel preparation requires a nuanced approach, prioritizing fluid balance and cardiac workload. Nurses must educate patients about the large volume of fluid involved and the potential for fluid overload, which can strain a compromised cardiovascular system.
Patients should be advised to report any symptoms of heart failure, such as increased shortness of breath, chest pain, or swelling in the extremities. The nurse should collaborate with the physician to consider splitting the PEG dose or utilizing a lower volume preparation if appropriate.

Close monitoring of vital signs, including heart rate and blood pressure, is essential throughout the cleansing process. Careful assessment and individualized planning are paramount to minimize cardiovascular risk.
PEG for Elderly Patients
Nurses instructing elderly patients on PEG bowel preparation must emphasize careful monitoring due to age-related physiological changes. Older adults are more susceptible to electrolyte imbalances and dehydration, necessitating slower administration and vigilant assessment of fluid status.
Clear, simplified instructions are crucial, as cognitive impairment can affect comprehension. Family members or caregivers should be included in the education process to ensure adherence and support. The nurse should inquire about pre-existing conditions, such as renal insufficiency or heart failure, which may require dose adjustments.
Encourage frequent sips of clear liquids and closely observe for signs of weakness, dizziness, or confusion. Prioritize patient comfort and address any concerns promptly to optimize safety and effectiveness.

Effectiveness of PEG with Ascorbic Acid
Recent research, notably from Healio, confirms that combining polyethylene glycol with ascorbic acid significantly enhances bowel cleansing efficacy for colonoscopy preparation.
Benefits of Adding Ascorbic Acid
Ascorbic acid, commonly known as Vitamin C, offers several advantages when incorporated into a polyethylene glycol (PEG) bowel cleansing regimen. As highlighted by studies reported on Healio, the addition of ascorbic acid demonstrably improves the quality of bowel preparation, leading to enhanced visualization during colonoscopy.
This improved clarity allows the physician to more accurately detect polyps or other abnormalities within the colon, potentially leading to earlier diagnosis and treatment. Patients are often instructed that ascorbic acid acts as an antioxidant, potentially reducing inflammation within the bowel during the cleansing process.
Furthermore, some research suggests ascorbic acid may help mitigate some of the common side effects associated with PEG solutions, such as bloating and nausea, although this requires further investigation. The nurse will emphasize that while generally well-tolerated, any unusual symptoms should be reported immediately.
Research Findings on PEG-Ascorbic Acid Combinations
Recent research, notably detailed in publications referenced by Healio, consistently demonstrates the superior efficacy of polyethylene glycol (PEG) solutions when combined with ascorbic acid for bowel preparation. Studies indicate a statistically significant improvement in colonic cleanliness scores compared to PEG alone.
These findings suggest that the ascorbic acid enhances the cleansing action of PEG, resulting in a greater proportion of patients achieving “adequate” preparation levels – crucial for successful polyp detection during colonoscopy. Investigations have explored various dosages of ascorbic acid, identifying optimal levels for maximizing benefit without increasing adverse effects.
Furthermore, research suggests a potential correlation between improved preparation quality and reduced need for repeat colonoscopies due to inadequate visualization. Nurses should inform patients that these combinations are increasingly favored due to their proven effectiveness.
Post-Cleansing Instructions
Nurses advise a gradual return to a normal diet post-PEG cleanse, resuming medications as prescribed, and promptly reporting any concerning symptoms to healthcare providers.
Resuming Normal Diet
After completing the polyethylene glycol (PEG) bowel cleansing preparation, it’s essential to reintroduce food gradually. Begin with clear liquids like broth, clear juice, and water to assess tolerance. Avoid red or purple-colored beverages, as they can mimic blood in the stool, causing unnecessary alarm.
As tolerated, slowly progress to easily digestible foods such as crackers, toast, bananas, and rice. Avoid high-fiber foods, fatty foods, and dairy products initially, as these can be difficult to digest and may cause discomfort.
Listen to your body and increase food intake incrementally over the next 24-48 hours. A bland diet is recommended initially, gradually expanding to your usual eating habits as bowel function normalizes. Staying hydrated is also crucial during this phase.
Medication Resumption
Importantly, discuss resuming your regular medications with your healthcare provider following the PEG bowel cleansing procedure. Certain medications, particularly those affecting kidney function or blood clotting, may require adjusted timing or dosage.
If you take medications for diabetes, blood pressure, or heart conditions, closely monitor your levels after resuming them, as bowel cleansing can temporarily alter their absorption and effectiveness.
Nonsteroidal anti-inflammatory drugs (NSAIDs) should be avoided initially, as they can increase the risk of bleeding. Always follow your doctor’s specific instructions regarding medication resumption to ensure your safety and optimal health outcomes post-procedure.
Follow-up Care
Following PEG bowel cleansing, schedule a follow-up appointment with your physician to discuss the results of your colonoscopy and any necessary further investigations or treatment plans. It’s crucial to address any lingering concerns or questions you may have regarding the procedure or your overall health.
Report any persistent symptoms like severe abdominal pain, fever, or rectal bleeding to your healthcare provider immediately. These could indicate complications requiring prompt attention;
Maintain adequate hydration and a balanced diet to support your recovery. Adhering to recommended screening schedules for colorectal cancer is vital for long-term health maintenance, as emphasized by medical professionals.